Hi there, we are Julie and Ciara and we represent the Northern Territory on the Executive of the Allied Health, Science and Technology Council of CSANZ. We both hail from Ireland, completing our BSc in Clinical Measurement Science in 2009 and 2012 respectively. Julie moved to Darwin in 2012, Ciara followed in 2016. We both completed International Board of Heart Rhythm Examiners certification in Ireland, and in Australia, Julie continued her studies to specialise in Echocardiography and Ciara specialised in Electrophysiology.
Since arriving in the Territory, we have both worked for NT Cardiac at Darwin Private Hospital (DPH), as Cardiac Physiologists. NT Cardiac services both private and public patients, across DPH as well as Royal Darwin Public Hospital. DPH has a Catheterisation Lab, where up to five pacemaker / defibrillator devices are implanted per week. Up until very recently, we had a dedicated day for Electrophysiology studies and ablations (Radiofrequency, Cryoablation and 3D Mapping). Unfortunately, this service is temporarily suspended as there is no Electrophysiologist available in the NT.
As part of our role, we service over 25 remote NT communities as part of a multidisciplinary team, consisting of a cardiologist, registrar, cardiac nurse, sonographer and sometimes a pacing trained Cardiac Physiologist. We have assisted with the implementation of new Cardiac Physiologist-led remote pacing clinics, designed to provide a greater level/continuity of service to patients and to ease the burden on the cardiologists on their one or two day remote trips.
Remote clinics present many challenges, some unavoidable. Many communities are often cut off from larger clinics in Darwin for months at a time during the wet season due to flooding. The larger community clinics like Katherine or Nhulunbuy are visited multiple times a year by the multidisciplinary team, however, some more remote clinics might have only 1 visit per year. As a result, providing optimal cardiac management to these patients can be difficult, compounded by the fact that some patients live in different communities depending on the season (wet versus dry season). Our visits sometimes coincide with funerals, cultural ceremonies or sorry business in the local community, which we always try our best to work around.
To accommodate these challenges, we schedule our pacing patients on a six monthly basis. Ciara has set up a list of patients at each community, and we aim to ensure at least yearly follow-up. Some patients are provided with home monitors at implant or follow-up, this enables us to receive data from remote locations to save medivac flights to Darwin. Remote community patients often lack access to Wi-Fi, often have limited mobile phone signal or access to mobile phones, and possibly intermittent electricity. For this reason, the majority of remote patients have their home monitors left permanently in the community clinic to send information to our clinic in Darwin. This puts added pressure on local dedicated staff that are already extremely busy, but these home monitors become highly useful in the case of emergencies.
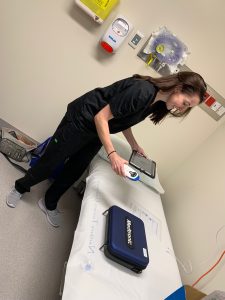 Providing echocardiography services to these patients also comes with its challenges. There can be limited facilities available at some clinics, with a lack of adjustable beds and adjustable trolleys for the echo machines. Room availability can be an issue, as there can be multiple visiting teams at the clinic at the one time. We scan a high volume of difficult pathology patients, for example double and triple valve replacements, all of whom are scanned on a portable machine. Patients can often be quite reluctant to come to Darwin, so these echoes in community are potentially their only follow-up scans.
Providing echocardiography services to these patients also comes with its challenges. There can be limited facilities available at some clinics, with a lack of adjustable beds and adjustable trolleys for the echo machines. Room availability can be an issue, as there can be multiple visiting teams at the clinic at the one time. We scan a high volume of difficult pathology patients, for example double and triple valve replacements, all of whom are scanned on a portable machine. Patients can often be quite reluctant to come to Darwin, so these echoes in community are potentially their only follow-up scans.
Despite the challenges, the Territory provides a hugely rewarding and unique working experience for allied health professionals. Our remote trips are a wonderful way to experience the NT and to see Territory life from a very different perspective and are a great opportunity to get to know your working team. It provides us with a great opportunity to try to improve systems, protocols and procedures, and therefore make a real impact to healthcare for our patients who live remotely.
Ciara Devoy, Cardiac Physiologist Julianne Pfister, Sonographer
Article recently published in the April On the Pulse – read in full here.


