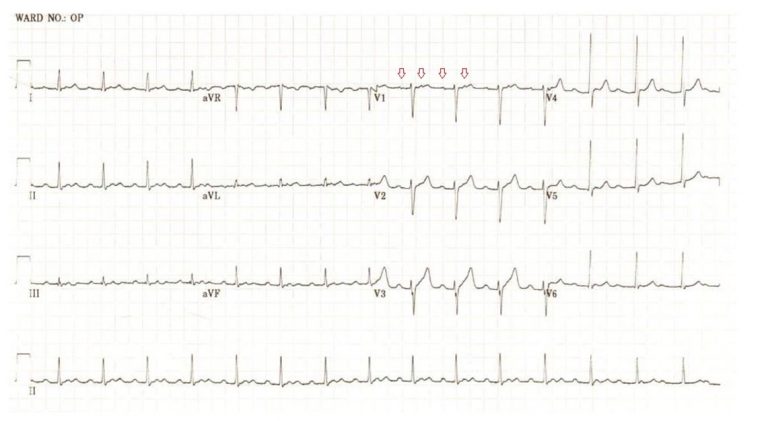
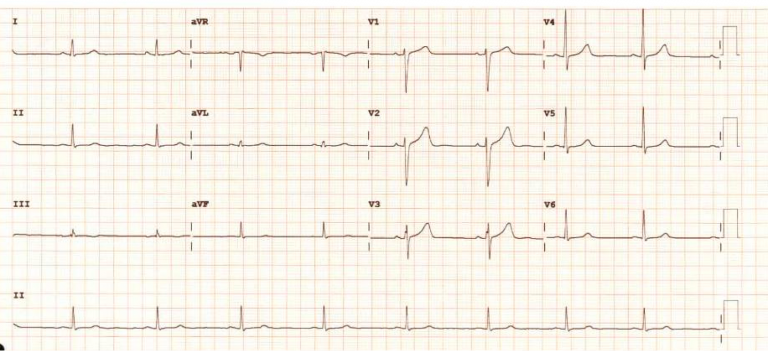
A 48 year-old male presents with 3 months of exertional dyspnoea.
He takes candesartan 8 mg daily and atenolol 50 mg daily for hypertension. ECG is shown above (Fig 1).
What is the most likely diagnosis?
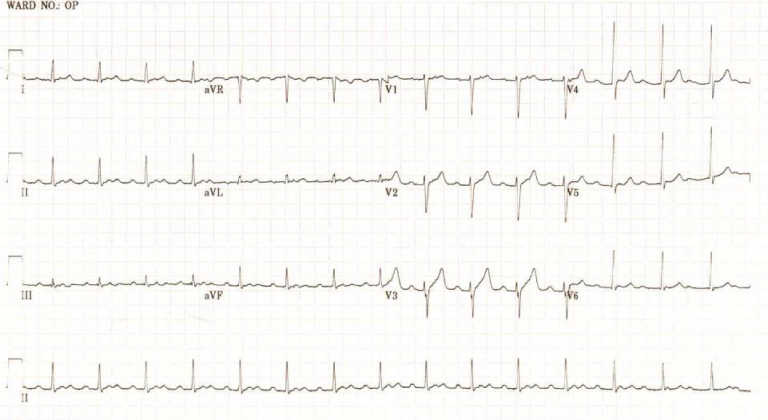
This patient was originally diagnosed with sinus tachycardia at 100 bpm.
In fact this patient has a focal atrial tachycardia originating from the right upper pulmonary vein (ECG following ablation shown in Figure 3). Atrial flutter or atrial tachycardia with 2:1 conduction (the start of the ECG) are often misdiagnosed as sinus tachycardia. There are two important signs that should make one suspicious that this is not sinus rhythm. Firstly, the presence of a long apparent PR interval would be unusual for sinus tachycardia in a young patient whereby elevated sympathetic tone would ensure more slick conduction down the AV node. Secondly, ‘funny’ appearance of T-waves should make one suspicious that there are P waves buried within them. Looking at all leads, particularly V1 (Figure 2) and mapping them out is instructive.