Pulmonary Hypertension in Aortic Regurgitation
by Dr Seshika Ratwatte
Pulmonary hypertension (PHT) is known to complicate left heart diseases (LHD) including left sided valvular pathologies such as aortic regurgitation (AR). Patients with significant AR have an increased risk of death, even if they do not have symptoms, so identifying variables which predict adverse outcomes is important. PHT is thought to develop in AR due to left ventricular volume overload which eventually leads to increases in left atrial pressure and the development of post-capillary PHT.
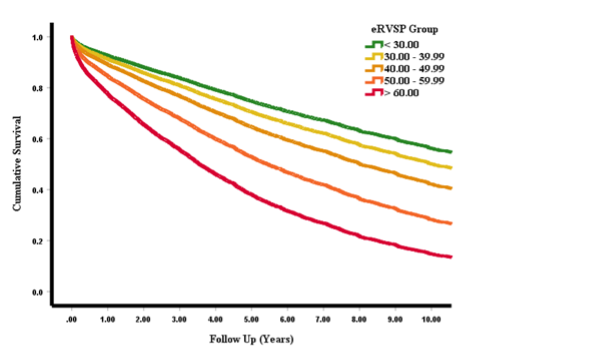
Now published in BMJ Heart, Dr Seshika Ratwatte, senior author Professor David Celermajer and their co-authors identify a cohort of 8392 patients with “isolated” moderate or severe AR and preserved left ventricular ejection fraction (LVEF>50%) using the National Echo Database of Australia (NEDA). The authors show that the risk of all-cause mortality increases as eRVSP level increases even after adjustment for age and sex (Central Illustration), with a ‘threshold’ for mortality seen from mild PHT onwards.
The publication outlines that a significant proportion of the population with significant AR had suspected PHT based on echo. Echo remains the first line screening tool to detect PHT and is the guideline recommended diagnostic method of choice to allow for monitoring and follow up. Clinicians need clear parameters to monitor and prognosticate such patients accurately. The authors identified a typical phenotype of “left heart disease” on echo with E:e’, right and left atrial sizes and the proportion of patients with RV functional impairments increasing progressively, from no PHT to severe PHT.
Central Illustration:
Link to publication is now available in BMJ Heart. https://heart.bmj.com/content/early/2023/04/02/heartjnl-2022-322187